Veterans Affairs leaders publicly unveiled their initial plans for coronavirus vaccine distribution this week as active cases and deaths related to the illness reached record highs among the department’s patients.
According to data publicly released by the department, officials at 140 medical sites across the country were tracking at least 17,629 patients with active cases as of Friday morning. That’s the highest daily figure reported by VA since the start of the pandemic, an increase of 188 percent from Nov. 1 and up 429 percent from Oct. 1.
In addition, VA researchers reported 446 deaths over the last week, the highest total of any seven-day stretch since the first VA patient died from coronavirus complications in mid-March. At least 5,542 patients have died from virus-related issues over the last nine months, an average of almost 21 a day.
In addition, at least 79 VA workers have died from the virus over that span. VA officials have declined to answer questions on how many of those were front-line health care workers who had direct contact with veterans.
RELATED
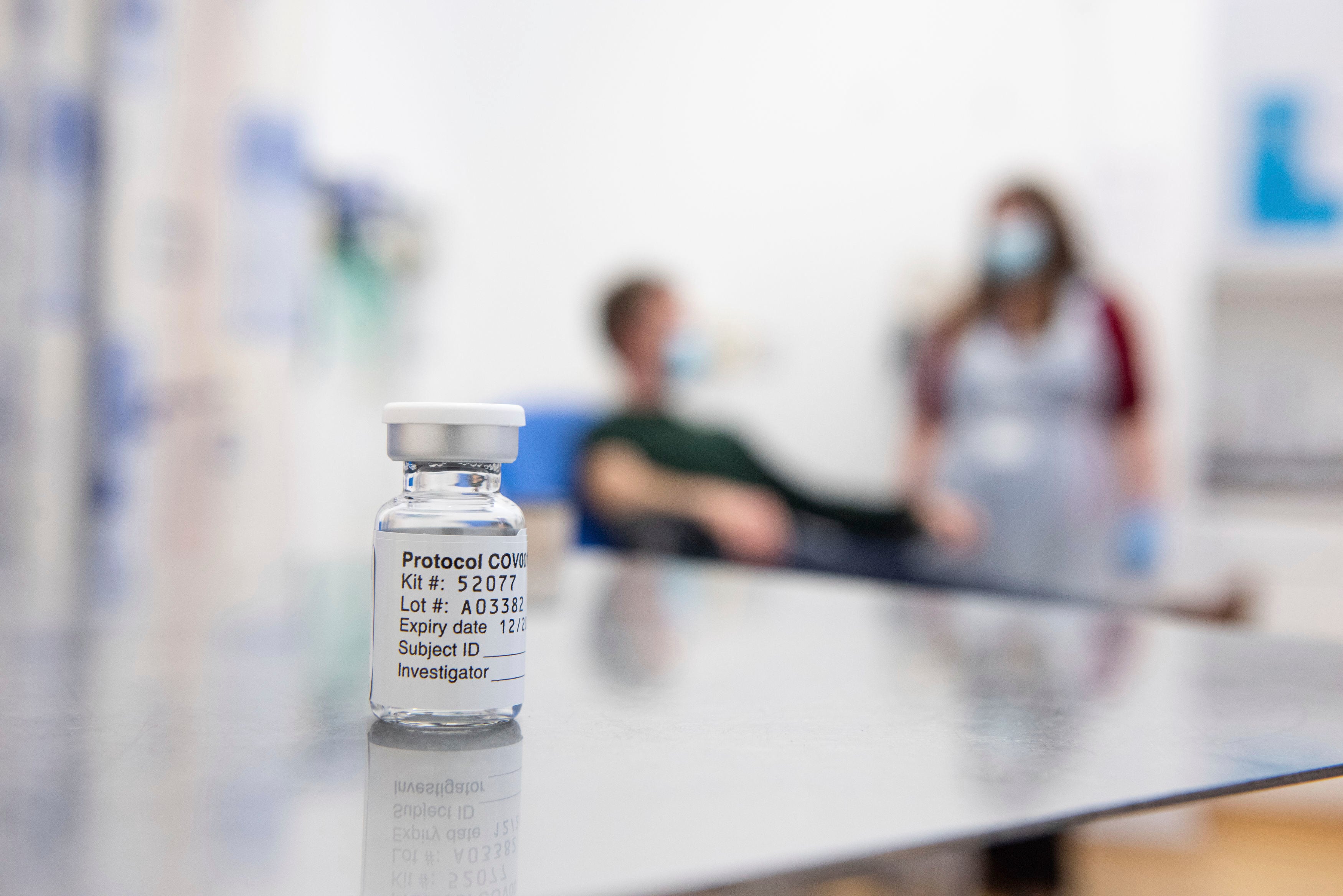
However, department officials have downplayed the sharp spike in case and death numbers over the last few months, saying that hospitalization rates among coronavirus patients have remained steady or declined.
The number of inpatients with the virus has also steadily increased in recent weeks, up about 255 percent since mid-October.
On Thursday, VA officials said they will begin providing vaccinations in coming days to front-line VA health care workers and veterans living in long-term care units at 37 of medical centers across the country. That work is contingent on final authorization from the Food and Drug Administration on vaccine use.
A day earlier, Richard Stone — the Veterans Health Administration’s executive in charge — told Senate lawmakers that about 73,000 doses would be available in the first wave of vaccinations. That’s enough to cover about 36,500 individuals, since the vaccine is a two-dose regimen.
In a statement, VA Secretary Robert Wilkie said that the department “is well prepared and positioned to begin COVID-19 vaccinations” and that “our ultimate goal is to offer it to all veterans and employees who want to be vaccinated.”
Priority will be given to health care workers “because they are at high risk for contracting and spreading COVID-19 to other staff members and patients.”
As more doses become available, department officials said, priority will be given to veterans “based on factors such as age, existing health problems and other considerations that increase the risk of severe illness or death from COVID-19.”
The initial 37 sites selected for the vaccines were chosen for their ability to reach a large number of veterans and ability to store the doses at extremely cold temperatures. The first vaccine, made by the pharmaceutical company Pfizer, requires refrigeration at temperatures of -70 degrees Celsius to remain viable.
RELATED
Those 37 sites are:
* Birmingham VA Health Care System (Alabama)
* Phoenix VA Health Care System (Arizona)
* West Los Angeles VA Health Care System (California)
* Palo Alto VA Health Care System (California)
* Eastern Colorado VA Health Care System (Colorado)
* West Haven VA Health Care System (Connecticut)
* Washington DC VA Health Care System
* Orlando VA Health Care System (Florida)
* Augusta VA Health Care System (Georgia)
* Edward J. Hines Jr. VA Hospital (Illinois)
* Lexington VA Health Care System (Kentucky)
* Southeast Louisiana VA Health Care System (Louisiana)
* Maryland VA Health Care System (Maryland)
* Bedford VA Health Care System (Massachusetts)
* Ann Arbor VA Health Care System (Michigan)
* Minneapolis VA Health Care System (Minnesota)
* Harry S Truman Memorial Veterans Hospital (Missouri)
* St. Louis VA Health Care System (Missouri)
* Omaha VA Health Care System (Nebraska)
* Southern Nevada VA Health Care System (Nevada)
* Raymond G. Murphy VA Health Care System (New Mexico)
* New York Harbor VA Health Care System
* Western New York VA Health Care System
* Durham VA Health Care System (North Carolina)
* Cleveland VA Health Care System (Ohio)
* Oklahoma City VA Health Care System (Oklahoma)
* Portland VA Health Care System (Oregon)
* Corporal Michael J. Crescenz VA Medical Center (Pennsylvania)
* Pittsburgh VA Health Care System (Pennsylvania)
* Caribbean VA Health Care System (Puerto Rico)
* Memphis VA Health Care System (Tennessee)
* Dallas VA Medical Center (Texas)
* Michael E. DeBakey VA Health Care System (Texas)
* Audie L. Murphy VA Hospital (Texas)
* Richmond VA Health Care System (Virginia)
* Puget Sound VA Health Care System (Washington)
* Milwaukee VA Health Care System (Wisconsin)
RELATED

Stone said he expects more sites to be added as new refrigeration equipment is installed, and as subsequent vaccines that do not require the extreme cold temperatures are approved.
More information on the vaccine distribution is available on the VA website.
Leo covers Congress, Veterans Affairs and the White House for Military Times. He has covered Washington, D.C. since 2004, focusing on military personnel and veterans policies. His work has earned numerous honors, including a 2009 Polk award, a 2010 National Headliner Award, the IAVA Leadership in Journalism award and the VFW News Media award.
