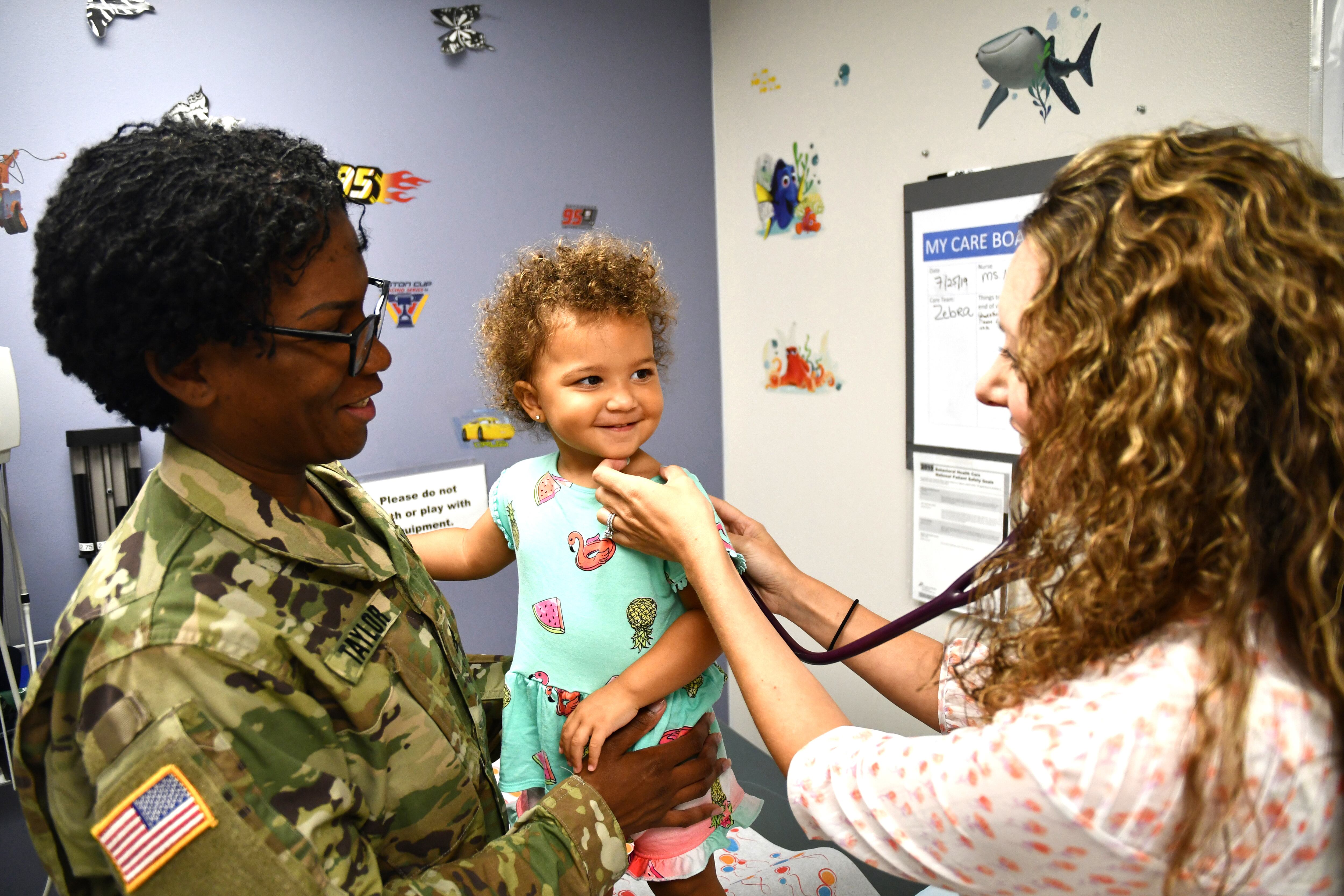
Military medicine may be at a turning point as it becomes increasingly affected by many of the same issues, such as shortages, facing the entire United States medical community, said the new director of the Defense Health Agency.
“We have to acknowledge that we’re part of an ecosystem, so if the United States is going to be short 250,000 to 300,000 nurses, which is a projection, that forces the health care system to look very hard at a model that is dependent on nurses,” said Lt. Gen. Telita Crosland, director of the Defense Health Agency, in a Jan. 20 interview with Military Times and other media.
“Nurses are everywhere in our health care system,” Crosland added, referencing practitioners ranging from operating and emergency room nurses to case managers and advice lines staff. “We have to look hard at our model of care.”
Crosland noted that she wants to examine models of how the military medical system can deliver quality care from the perspective of the patient.
“I think we have a great opportunity with innovation,” she said. “The pandemic showed us that in a crisis, the adoption rate of virtual care went to levels none of us would have predicted.”
Virtual health care is likely to expand in the U.S. at large, as well as in the military. If officials are able to push more care into the home, and put more care into the hands of the patient, those patients “have more stake in it, they have more control, and that might be the best value proposition for the entire system,” Crosland said.
RELATED

Doing so boils down to improving access to quality health care. That’s been a perennial issue for military families, especially in certain locations. And families are letting their leaders know about it.
Secretary of the Army Christine Wormuth told soldiers and families during a Jan. 24 town hall meeting in Hawaii that everywhere she goes, she hears requests for more access to doctors. She said it’s particularly difficult in relatively remote areas like Fort Irwin, California, where a procedure like a mammogram is not available on post.
“It’s hard to attract doctors to Fort Irwin because of the very, very long distances that are involved,” Wormuth said.
Wormuth also cited “real challenges” with the ongoing national shortage of behavioral health resources.
“We all need more,” she said. “I want to work more with our medical community to do what we can to try to increase the resources that are available.”
An emergency room nurse at Tripler Army Medical Center had asked Wormuth whether there were any plans to increase the number of psychiatrists and psychologists at Tripler, especially for children. She specifically mentioned the Exceptional Family Member Program, where more resources are needed. The nurse, who works with patients from all the service branches, said it’s “really an issue that I’ve seen first hand.”
Across the country and in a variety of medical professions, Wormuth said, there’s a lot of burnout and other issues. The pandemic has stressed medical professionals throughout the country.
“We’ve got to get on top of [the issues] or we’re not going to be able to recruit people into the medical profession in the numbers that we need,” Wormuth said.
Karen has covered military families, quality of life and consumer issues for Military Times for more than 30 years, and is co-author of a chapter on media coverage of military families in the book "A Battle Plan for Supporting Military Families." She previously worked for newspapers in Guam, Norfolk, Jacksonville, Fla., and Athens, Ga.