This story is part of the portfolio that won the 2023 Society for Professional Journalists Dateline Award for beat reporting in a newsletter or trade publication.
Capt. Carlos Mendoza wanted to do his laundry.
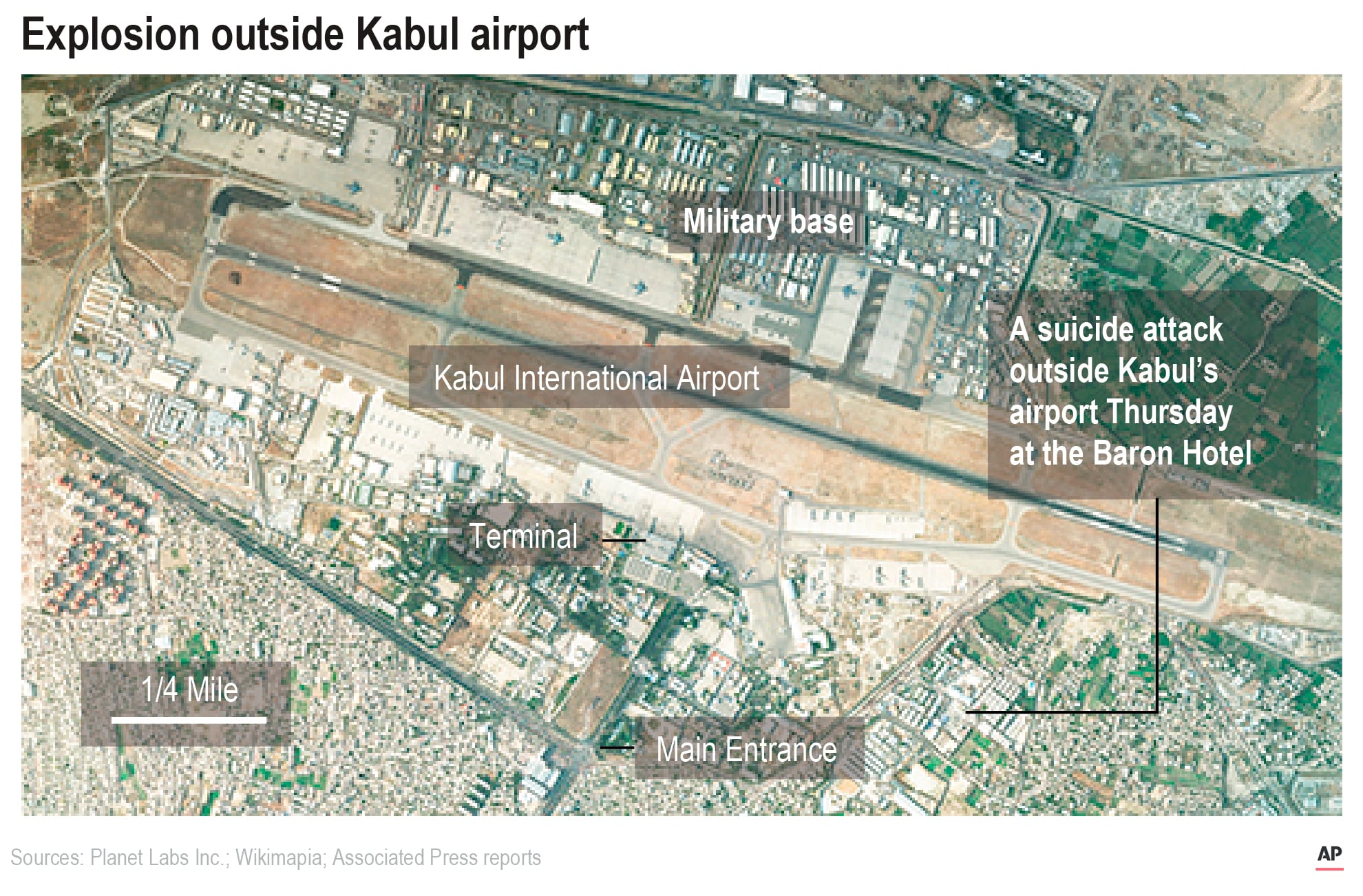
It was the morning of Aug. 26, 2021, at Hamid Karzai International Airport in Kabul, Afghanistan, where Mendoza had been awake for nearly 24 hours thanks to his nighttime shift as a flight nurse during Operation Allies Refuge — the massive U.S.-led humanitarian effort to help Afghans escape the resurgent Taliban.
After a week of nonstop operations in Kabul, this was Mendoza’s chance for a fresh uniform. He thought he could squeeze in a load of clothes and — maybe, if he was lucky — some sleep.

He had napped for less than an hour when he awoke around 1 p.m. to the news that their facilities were under threat. So Mendoza headed to the hospital, the safest nearby building, to wait it out.
Then at 5:36 p.m., an Islamic State militant wearing about 20 pounds of explosives wedged himself into the desperate crowd outside the airport’s Abbey Gate and detonated the contraption.
Battered and burned victims needed Mendoza’s help. Rest would have to wait.
“It just kept coming and coming and coming,” Mendoza said of the wounded. “You’d stop for a minute to gather your thoughts … ‘What’s the next step?’ And then go, go, go, go, go again.”
Air Force Times exclusively spoke with five airmen who were assigned to the 379th Expeditionary Aeromedical Evacuation Squadron during Operation Allies Refuge. They were among the select few who cared for patients injured and killed in the attack on the airport’s Abbey Gate, on the front lines of the withdrawal’s most catastrophic 48 hours for American troops.
Thirteen U.S. service members and at least 160 Afghans died because of the suicide bombing. The death toll would have climbed higher if not for military medics, surgeons, medical specialists and logisticians.
“This squadron answered the call for OAR, it answered the call for the mass casualty event at the Abbey Gate, and serving as commander of this squadron is one of the proudest moments in my career,” said Lt. Col. Robert Huhn, who led the 379th EAES at the time.

‘I was holding his heart’
Rumors of a blast reached the hospital first, followed by a growing stream of casualties.
Staff Sgt. Morgan Reed, who handled communications for the aeromedical evacuation liaison team on the ground in Kabul, knew something was off when wounded Americans began coming through the doors — unusual in a sea of largely Afghan patients.
They arrived with wounded chests, spinal cords and tracheas. The explosion left them with major organ damage and traumatic brain injuries.
A few U.S. service members were still alive when they arrived, after standing close to the bomber.
Medical personnel saved the life of at least one American who was near death after rescuing a fellow Marine — an act that earned the man a Bronze Star, Mendoza said. The airmen declined to confirm patients’ names because of health privacy laws.
An Air Force doctor cut open the Marine’s chest, searching for the reason the patient couldn’t breathe. Finally, they discovered an elusive bleed on the man’s lung and hurried him into an operating room.
“I was holding up his ribcage … trying to expose as much as I could so the doctor could see it,” Mendoza said. “When I was holding his heart, I could see [it] slowly stop beating.”
Medical staff massaged the Marine’s heart. They transfused around 10 units, or 1.5 gallons of blood — about as much as is in an average adult’s body. His heartbeat slowly returned.

“Essentially, he died,” said Maj. Dominick Vitale, a physician on a critical care air transport team, who transported the Marine out of Afghanistan and noted he recovered well at Walter Reed National Military Medical Center. “The efforts on the ground ... brought him back to life.”
After surgery, Mendoza visited the Marine to clean the grime off his face. The captain soon learned his patient was awake and responsive.
“To find out later on that he did make it, and then to hear the stories of the things that he did for his fellow Marine, it makes you feel good about the efforts that you made that day — the pain and the things that you went through to get this stuff done,” Mendoza said.
Others fared worse. Reed stayed with one Marine as he died from brain swelling that was too severe to stop.
“We were doing our best,” Reed said. “We didn’t know if he could hear us or not, but we were trying to comfort [him] somewhat.”
Mendoza, on his way to get a tracheotomy tube to help another Marine breathe, overheard a nearby discussion of chaplains. He pointed them toward the dying American.
The Marine’s countrymen couldn’t save him. But they could administer his last rites.
Another American died on the operating table, Reed said. Medical staff worked with two soldiers manning the morgue to identify the deceased and put them in temporary body bags until their remains could return to the U.S.
‘Unregulated mission’
Alongside the Americans came the Afghans. Without the ability to communicate, patient paperwork, paper itself, or even names, they needed to think on their feet.
Medical staff at the Norway-run field hospital at first differentiated between patients by naming them after Norwegian mountains, then describing them by their injuries or other monikers, Mendoza said.
Troops treated the casualties anywhere they could find space. Any available vehicle became makeshift ambulances, shuttling medics, orphaned toddlers, or people who couldn’t walk, to the flight line and back for hours.
Mendoza and Reed made rounds to check on the patients’ statuses, set up the equipment needed to load those who were stable enough onto planes, tried to reunite Afghan family members, and met the jets as they landed.
Vitale was two hours into his own post-mission nap at Al Udeid Air Base, Qatar, when his team got word of the bombing. They scrambled to take off on a three-hour, “very pensive” flight, he said.
“This is what we call an ‘unregulated mission,’” Vitale said. “We don’t know how many people you’re going to get. We don’t know who they are, what their ages are, what their injuries are, but just be prepared for whatever you find when you get there.”
Thursday was becoming Friday by the time Vitale’s group arrived in Kabul. Critical care teams — a doctor, a respiratory therapist and a nurse — usually take on patients who stabilize over multiple days before flying to a new facility.
There, though, Vitale and his colleagues had to juggle 25 patients whose health was still tenuous and required “very intense management and troubleshooting” for several stressful hours in flight, he said. Six were wounded at Abbey Gate.
Patients bled in flight and struggled with low blood pressure and hypoxia, Vitale said. They had trouble with sedatives and lacked viable veins for intravenous infusions. They fought to breathe. And airmen only had so many medical supplies to go around.
“I don’t think, in the last 10 years, that anybody who was deployed in that environment was involved in anything similar or even close to combat-related missions. You’re flying into a hostile environment,” Vitale said.
Typical medevacs are pre-planned, with plenty of patient information available and with fewer at once. OAR was not that kind of operation.
The 379th sent a team to work out of the Kabul airport to help move a large influx of patients onto aircraft — a decision that came in handy on Aug. 26. The squadron brought in a few dozen more troops to support medical procedures, and airmen brushed up on a broad range of clinical care.
“Things were not necessarily going to occur as we’ve been trained to do traditionally,” Huhn said.
That prediction proved spot-on. A passenger experienced an in-flight medical emergency on nearly every C-17 Globemaster III that ferried Afghan evacuees out of Kabul, Huhn said, from childbirth to nausea and vomiting to fainting or a more traumatic injury. More than 79,000 people left the country on around 330 U.S. military flights from Aug. 11-31, 2021, the Air Force said.
Air Force medics began bringing a small medical backpack on board each passenger flight to better respond to those cases. Medics would treat some urgent conditions in flight if a situation couldn’t wait for a doctor at Al Udeid with the help of people who helped clear space on the plane and passengers who acted as translators.
“It was a very communal experience,” Huhn said. “Everyone was helping each other even though … you don’t know these people. They all understand the situation.”

The medical group at Al Udeid was overwhelmed by the avalanche of need arriving on the C-17s, so the medevac team set up a separate immediate care clinic to receive passengers as well. In total, the two clinics saw 7,300 patients in about seven weeks during Operation Allies Refuge.
Patients showed up with broken arms, heat exhaustion and bleeding leg wounds from “running from the Taliban for the last 10 days,” Huhn said. He estimated they saw about 200 pregnant refugees whose dehydration caused too-early contractions.
“Everybody leans on each other in these moments, where some people have more experience than others. Some people are more nervous and scared than others. But we talk to each other. … Everyone knows they have a job to do,” Vitale said.
In all, the team in Kabul treated around 60 patients in the Abbey Gate bombing’s aftermath. Most were evacuated for more comprehensive care.
From the time the suicide bomb went off to the last medevac departure, the airmen had been awake and moving for almost two days straight.
“We put in, like, 46 hours of work, [in] two missions, over three time zones,” Vitale said. “It was definitely a day I don’t think any of us will really ever forget.”
Reed’s watch logged 15 miles of running around the hospital and to the aircraft. Mendoza peeled off socks that had melded to his feet. They’d barely eaten.
Three days later, they were gone.
Rachel Cohen is the editor of Air Force Times. She joined the publication as its senior reporter in March 2021. Her work has appeared in the Washington Post, the Frederick News-Post (Md.), Air and Space Forces Magazine, Inside Defense, Inside Health Policy and elsewhere.





