COEUR D’ALENE, Idaho – When the 12-hour-plus workday is done, the 20 Army nurses and doctors deployed to this scenic town leave a civilian hospital overrun by COVID and carry the weight of the shift back to their hotel.
For Capt. Corrine Brown, an intensive care unit nurse, that burden involves the uncertainty that remains when treating the sick, 19 months after the pandemic changed everything.
“COVID doesn’t act like any other disease that we’ve previously treated,” Brown told Military Times this month between sips of Gatorade during a break in her shift. “It’s almost like dealer’s choice if they’re going to get better or get worse.”
Brown and her military colleagues are last-gasp reinforcements here, sent in via the Federal Emergency Management Agency a few months ago to help with a ceaseless conveyor belt of sickness that threatened to break Kootenai hospital.
It’s a once-unprecedented military mobilization that has steadily become the norm during the pandemic.
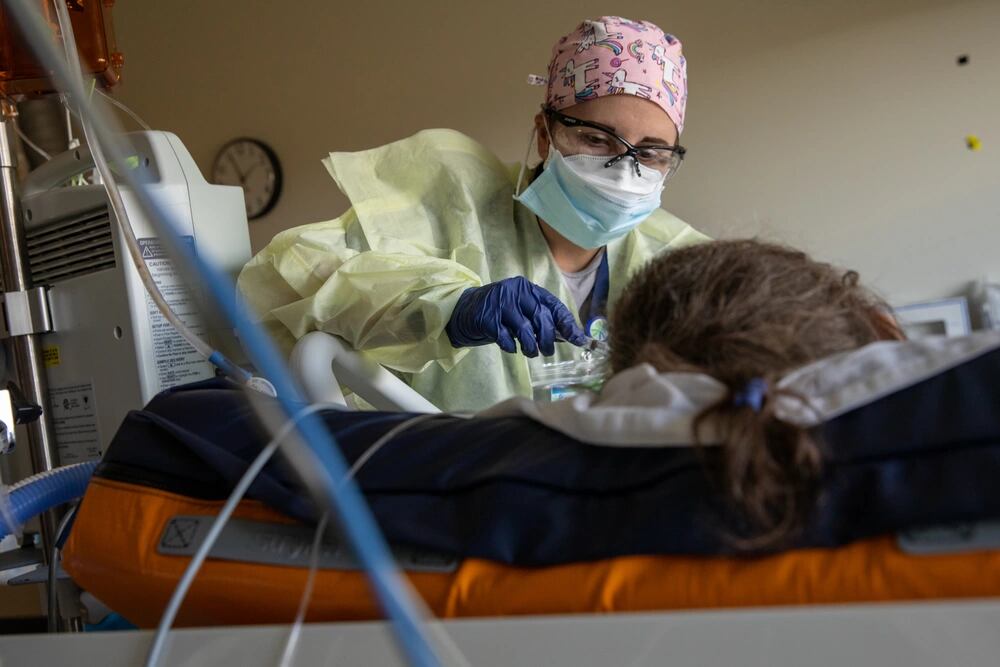
The crush of cases here is born of a population as skeptical of COVID and masks as the nearby Lake Coeur d’Alene is wide. And after hours, other Army nurses here linger on the bafflement of patients who didn’t believe in the disease, got infected, couldn’t breathe and ended up hospitalized.
“Because the number of unvaccinated patients that we see is so high, and they feel so misinformed when they get the infection…it’s this thing that they’ve never thought about and now they are in a very critical state,” Army Capt. Jason Webb, another ICU nurse, said earlier this month. “People are still shocked when they get this infection and when they get so sick. And it kind of perplexes me that that’s the case.”
Even as the cases keep coming and the state enacts crisis standards of care to deal with the flood, life outside continues as if no pandemic exists.
Just 46 percent of Idaho residents are fully vaccinated, according to state data, nearly 30 points below the national percentage of fully vaccinated adults.
As the pandemic trudges on here, any talk of COVID mitigation—such as requiring masks—has been met with an increasingly aggressive edge.
A local school district axed plans for a mask mandate after hundreds of protesters swarmed a school board meeting last month and then descended on the district headquarters, prompting a lockdown, The Associated Press reported.
These attitudes have left hospital staff to deal with infection largely on their own, even as they face local ire themselves.
“We have had people show up with video cameras to be greeted by security, to then cuss them out and call them sheep, then post the video to YouTube,” Caiti Bobbitt, a hospital spokeswoman, said. “Family members yelling at staff for not giving alternative treatments. Family members yelling at staff for killing their loved ones because COVID isn’t real.”
Amidst this fevered swirl, the Army team and their civilian counterparts work away, trying to save lives.
“I would love to see this community not in crisis,” Brown said.
RELATED
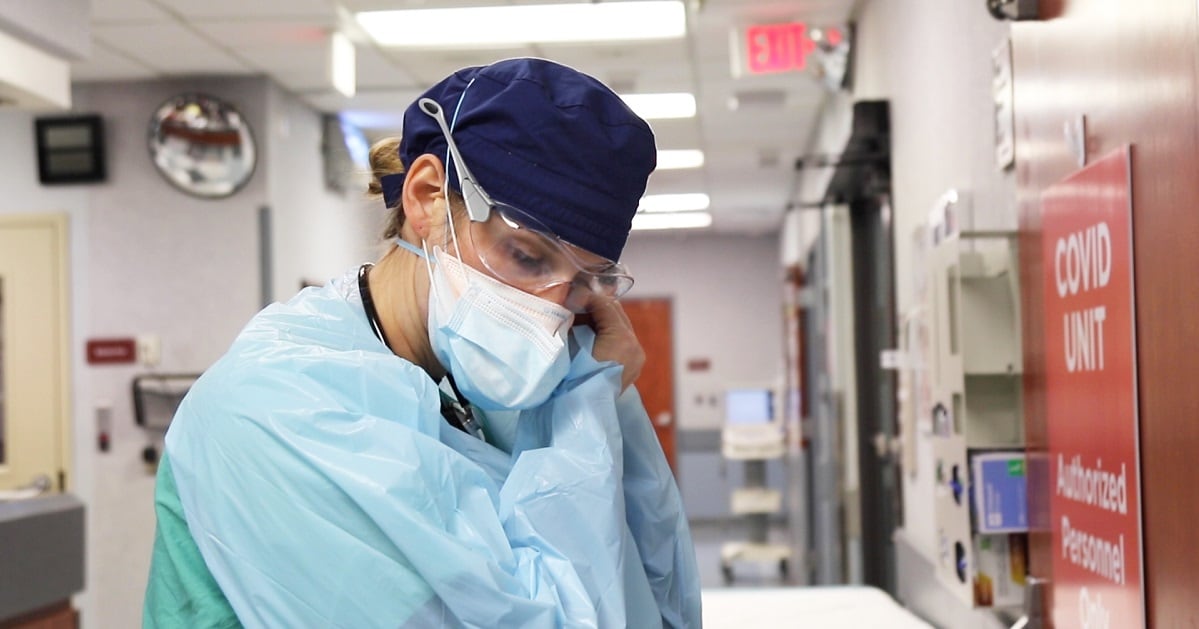
Across America, military medical troops like Webb, Brown and the rest of the Idaho team have been a lifeline throughout the pandemic for civilian hospitals like Kootenai.
To date, nearly 5,000 troops have fanned out to COVID hotspots in 19 states and 60 cities, helping overwhelmed staff at 81 hospitals deal with the deluge since March 2020.
Just since August, roughly 200 Army, Air Force and Navy medical providers have deployed to the nation’s hardest hit regions, including Idaho, Alabama, Mississippi, Tennessee and Louisiana to help with waves propelled along by the Delta variant and low vaccination rates.
It’s a far cry from the traditional combat medicine duties of the Idaho team’s unit, the 10th Field Hospital, out of Fort Carson, Colorado, and military medical troops generally don’t provide care to civilians.
But these are unprecedented times, and several of the Army medical staff deployed to Kootenai reported treating past COVID surges from California to Texas.
Several of the Idaho Army team said they never thought they’d take on such a mission.
“It’s just a really high level of stress, constantly,” Brown said. “Your brain just doesn’t stop…we want to support the people of this community so much.”
‘A very hard place to work’
Following a weekly press conference outside the Kootenai hospital on Oct. 6, during which officials noted there had been one COVID death each day in the young month, the patient numbers continued to swell.
All told, the hospital had 150 COVID patients that day, and had opened overflow areas in the complex to accommodate the sick.

As of Monday morning, the hospital was reporting 128 COVID patients, 40 of whom required the ICU, a marginal improvement.
Still, this latest wave has pushed the hospital at times to run 50 to 60 ICU patients a day for an ICU ward normally licensed for just 26 beds.
Earlier in the pandemic, the hospital had dealt with more manageable influxes that peaked around 94 patients, according to hospital officials, who requested help from the Federal Emergency Management Agency in August.
Civilian and military medical officials said the crisis was made worse by low COVID vaccine take rates and no government-mandated mitigation, like requiring masks indoors.
Even among the civilian hospital staff, vaccination rates hover at about 50 percent, and even some physicians remain skeptical of the jab, Dr. Robert Scoggins, chief of staff for critical care, told Military Times.
Vaccine attitudes have led to splintering among the hospital staff, he said.
“It’s a very hard place to work right now,” Scoggins said. “The patients are very sick, and it’s constant. It’s just a constant struggle to take care of these patients on a daily basis. The nursing staff is tired.”
Idaho has a right-wing libertarian streak, and some nearby residents are distrustful of the government, which has confounded efforts to get buy-in for the fight against COVID, Scoggins added.
He blames the case numbers partly on social media, which has allowed false information about COVID and the vaccines to flourish.
Sometimes, Scoggins wonders if such hesitancy would have been around if COVID hit 20 years ago, before social media took over.
“We still find people skeptical even when they’re sick with COVID,” he said. “They don’t believe us, which is really tough.”
Scoggins said he wasn’t sure where they would be if it wasn’t for the Army doctors and nurses, who are there until early November.
The hospital has put in for an extension of federal assistance beyond that date, but as of Monday, they had not yet received an answer.
“I know it will end at some point, I think the numbers will eventually go down, I just don’t know when that’s going to happen,” Scoggins said.

‘He never recovered’
Kootenai has a no-media policy for areas of the hospital where COVID patients are treated.
But on Oct. 6, several of the deployed Army team, face-masked and bleary eyed, took a break from the workday to share their experience with Military Times.
Asked to describe her craziest shift of the deployment, Capt. Brown, the ICU nurse, laughed dryly and answered, “this morning.”
“Critical care nurses, our big thing is critical thinking, anticipating what’s going to happen next,” Brown explained. “Knowing, okay, based off their diagnosis and what medications they’re on, this is where I can expect things to go.”
But with COVID, predicting whether a patient is going to improve or die remains anybody’s guess.
“As of late, the last week or so, it’s been very quick declines, where they’re doing fine and everything seems to be okay,” Brown said.
Patient oxygen levels are fragile, and that vital indicator sometimes drops with the slightest movement.
“It just takes one event, one time for them to…get up and move around, and their oxygen will crash…to a place where it can’t recover,” she said.
“That’s actually what happened to our patient yesterday,” Brown added. “All we were doing was…just shifting them. We shift them every two hours to make sure they don’t get bed sores, and we were just doing a shift and it just moved things…and it must have taken just a little bit too much of his oxygen demand.”
“He just never recovered from it.”
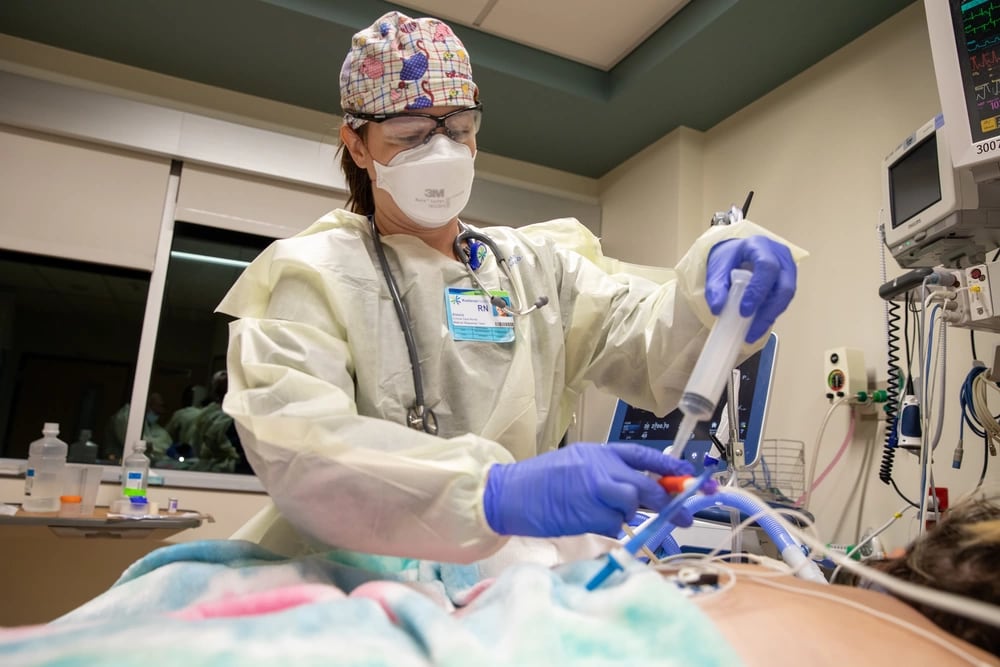
Webb likened the illness to being held underwater.
“You take the oxygen off so they can blow their nose or whatever and all of a sudden they’re basically suffocating,” he said. “It’s terribly frightening…You can provide all the medical education in the world, but that does little to sway the fears of dying from a lack of oxygen.”
Three nurses are assigned to every six patients in Kootenai’s COVID ICU. Keeping tabs on everyone’s vitals and medications is time-consuming in and of itself before a patient’s condition worsens.
“Yesterday and today, honestly, we’ve had patients that were so sick…we were completely maxing them out on the oxygen support that we can give them, the blood pressure support we can give them, medications that artificially kind of raise their blood pressure in order to make sure they’re still (supplying oxygen to) their vital organs, their brain, their heart, their lungs,” Brown recalled. “We had three patients that were kind of at that point yesterday on our team alone.”
She also noted a recent patient whose blood pressure continued to plummet, and how she and other providers worked on that patient for three hours.
“We hung five different types of medications on one patient in an hour, just trying to keep their blood pressure up enough to where they’re (supplying oxygen to) their brain, so they don’t get brain injuries,” Brown said.
This unpredictability leaves medical staff unable to reassure loved ones of the sick, according to Webb.
“They say, ‘when is he or she going to get better?’” he said. “And my answer is always going to be, ‘I don’t know when that’s going to be or even if they’re going to get better, and they may or may not get worse before they get better.’”
Webb said Oct. 5, the day before he spoke with a Military Times reporter, was the craziest, most hectic shift he had experienced.
“A patient that was already extremely sick got even sicker, we pulled out literally all the stops,” he recalled. “In addition to that, I had…three other extremely sick patients and two other stable, very sick patients.”
“That was a very taxing day,” Webb added. “I went home and just slept.”
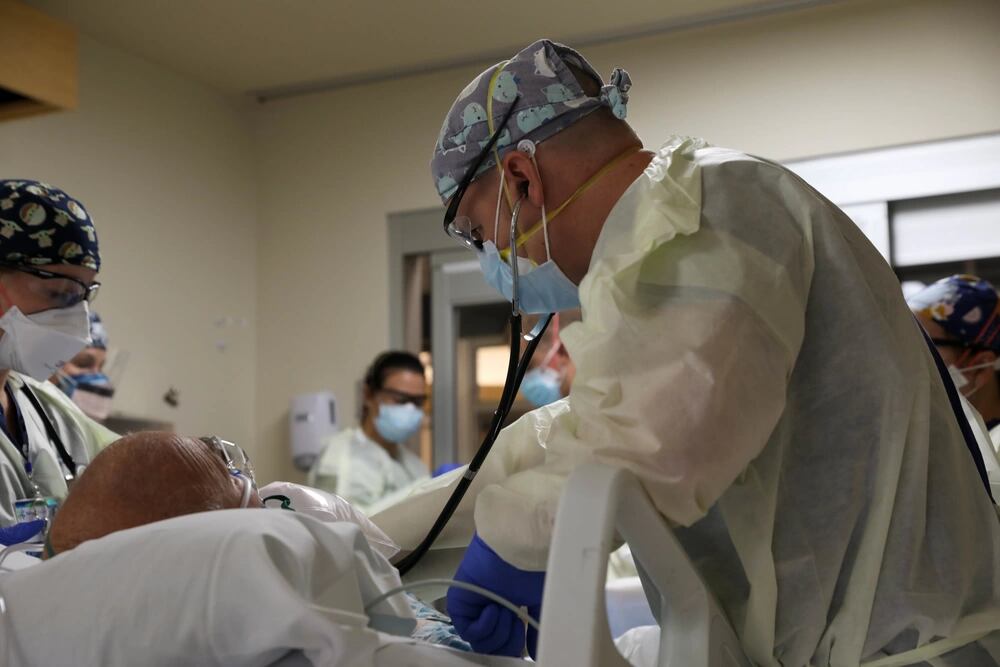
‘I’m just tired’
While all the Army medical men and women at Kootenai are emphatically pro-vaccination, Brown and the others said they’re not here to judge their patients’ attitudes on the issue.
Sometimes, patients are resistant to the treatment plan that will get them home, according to Capt. Nicole Barth, a nurse working in the hospital’s progressive care unit, one severity level below the ICU.
“They just don’t seem very grateful for care,” said Barth, who deployed to a civilian Los Angeles hospital earlier this year to help with a prior surge. “And they just are very obstinate to their treatment plan. And unfortunately, some of these patients, because they don’t want to follow their treatment, go to higher level care.”
Some patients will resist nurse entreaties for them to lie prone on their stomachs, a position that helps them breath.
“All we do is want them to feel better and get better,” Barth said. “It’s just so frustrating when patients don’t want to participate in their plan of care to leave the hospital.”
RELATED
Being hospitalized with COVID is isolating, Barth said, so she tries to make small talk with her patients and found that football is a unifying topic.
The disease makes her patients sleepy and fatigued, but they try to keep them awake during the daytime.
Some have difficulty talking because they get out of breath so easily, Barth added.
“Some patients can’t leave their bed because their oxygen dips way too much,” she said. “But some of them can walk a little bit…walk to the bathroom, but then they have to recover.”
Despite being winded from a trip to the bathroom, some patients are heartened by the fact they can walk at all.
“Once they move from the ICU to us, they’re just so thankful to walk to the bathroom,” Barth said. “That’s a huge feat for them. That’s such a good feat for the day…Two days ago, you couldn’t even stand up.”
During her deployment to Riverside hospital outside Los Angeles earlier this year, Barth said she often reflected on the day’s work.
“I would sit there and just think a lot,” she said. “But here, I’m just tired.”
Geoff is the managing editor of Military Times, but he still loves writing stories. He covered Iraq and Afghanistan extensively and was a reporter at the Chicago Tribune. He welcomes any and all kinds of tips at geoffz@militarytimes.com.




