Seaman Danyelle Luckey “didn’t die in combat or any military operation. She died from gross negligence of the medical providers on the ship she served, the USS Ronald Reagan,” said her father, Derrick Luckey.
Danyelle Luckey died from sepsis on Oct. 10, 2016. The 23-year-old had been on the ship for two weeks, and had been going back and forth to medical from Oct. 3 to Oct. 9 with worsening symptoms. “Her death was very preventable. She died in excruciating pain, instead of being properly treated,” Derrick Luckey told lawmakers during a hearing about patient safety and the quality of care in the military medical system.
“If the medical providers had given her a simple treatment of antibiotics instead of turning her away, she would be alive today,” he said.
Luckey and Army veteran Dez Del Barba, who said he lost part of his left leg and suffered 70% muscle and tissue damage after his strep infection went untreated, urged lawmakers to make changes so others in the military community don’t have to suffer.
Both contend this could have been avoided if proper medical care, such as antibiotics, had been provided. And both said they haven’t been able to get any information on investigations, or any actions to hold anyone accountable.
“My daughter’s career and her life were taken from her, while these people continue in their careers,” Luckey said.
“Those responsible for the medical care I received are still employed by the Army to treat more service members,” Del Barba said, referring to the care he received at Fort Benning, Ga.
Meanwhile, the Government Accountability Office has found found inconsistencies in military medical facilities’ procedures for verifying the credentials of medical providers, and in reviews of patient safety events that caused harm to patients or could have caused harm. These preliminary observations are the result of an ongoing review by GAO which is expected to be completed this summer.
“When our service members suffer from poor quality medical care, when doctors fail to provide the standard of care or woefully ignore symptoms or conditions, we need to make sure that there is a system in place to both prevent the incident from happening again and hold the providers accountable,” said Rep. Jackie Speier, D-Calif., chairwoman of the personnel subcommittee of the House Armed Services Committee.
After Luckey and Del Barba testified, Army Lt. Gen. Ronald Place, director of the Defense Health Agency, addressed them in his comments. “Your testimony today was compelling and heartbreaking. It’s clear that you suffered tremendous loss, and I take it very seriously when there are bad outcomes from the medical care provided within our system. …
“I’m deeply committed to ensure we learn from your losses so we can better our health care system, so we can have fewer losses. My goal is to make this health system stand as one of the finest, if not the finest, in the nation. Those who serve their country should expect that,” Place said.
“You have my word.”
Speier said she is frustrated that Department of Defense has been slow to implement the Stayskal Act that Congress included in the 2020 National Defense Authorization Act. The law allows service members to bring claims against the United States for injuries and deaths caused by improper medical care.
Luckey said he has learned that the claims are not allowed for damaging care that is received aboard Navy ships or at overseas military facilities.
Lawmakers will address this issue in legislation this year, Speier said. She said her efforts to allow service members to bring these claims aren’t just a matter of justice, but it’s about accountability.
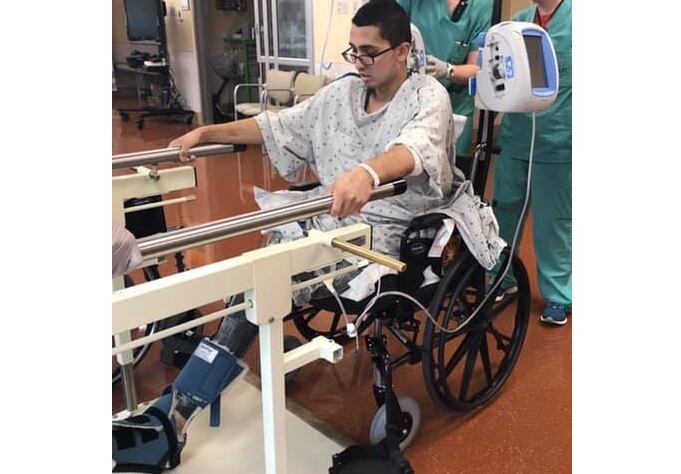
Dez Del Barba’s Army career was cut short when his strep throat was left untreated at Fort Benning, Ga., during basic combat training in 2019. He’d been accepted for Officer Candidate School. “It only took 35 days for the military to destroy my life,” he said. “I was left grossly neglected by the U.S. military health care system and by my basic training leadership at Fort Benning.” The illness progressed to necrotizing fasciitis, an infection of the skin and soft tissue. His left leg was amputated above the knee, and he’s undergone 43 surgeries and a number of skin grafts.
RELATED
“This was preventable. … It could have been avoided had the providers at Fort Benning given me adequate medical attention,” Del Barba said.
His medical record at Fort Benning is less than 100 pages, he said. Yet after three years and 19 days, the Army has no clear answers for him on the status of its Quality Assurance Investigation.
Del Barba said a strep test came back positive on a Friday, but the medical provider simply put a note in his record to notify him on Monday. Meanwhile, by that Sunday, Feb. 10, he was so ill a fellow soldier had to help him to sick call. The doctor prescribed throat lozenges and said his legs were sore due to running.
“That’s gross incompetence, and it shouldn’t take three years for a Quality Assurance Investigation,” Speier said.
Asked by Speier about what the Army has done in the wake of Del Barba’s case, Surgeon General of the Army Lt. Gen. Scott Dingle said investigations have been conducted.
The Army is focusing on “zero preventable harm in the delivery of medical care,” Dingle said.
Surgeon General of the Navy Rear Adm. Bruce Gillingham said the Navy has developed a fleet-wide sepsis screening, so that if a sailor reports to sick call aboard ship, the corpsman can use that screening tool to detect whether there are risk factors for that person to develop sepsis and a treatment protocol if sepsis is identified. The protocols have been shared with their military treatment facilities, too, he said.
The Navy has also deployed a Joint Patient Safety Reporting System across the fleet, he said.
Military medical facilities and the Defense Health Agency don’t always adhere to the agency’s credentialing and privileging of medical providers, said Sharon Silas, director of the health care team for the Government Accountability Office. She testified about preliminary observations of DoD’s monitoring of health care providers’ qualifications and competence.
Their preliminary results show, for example, the MTFs didn’t follow requirements to verify the medical licenses before granting practicing privileges to 16 out of 100 providers reviewed at four military treatment facilities. Silas noted that the Defense Health Agency is ramping up its monitoring of procedures in military treatment facilities.
“We don’t want practitioners out there providing services to our service members who either need more training, have forgotten their training, or just are not good physicians or health care professionals,” Speier said.
GAO found instances where military treatment facilities are not always following procedures in reviewing patient safety events that caused harm to patients, or could have caused harm. Lt. Gen. Place said for patient safety, DHA uses strategies and practices from the private sector and uses widely accepted measures for performance. “Over the last four years, DoD has seen improved patient safety performance,” he said.
Karen has covered military families, quality of life and consumer issues for Military Times for more than 30 years, and is co-author of a chapter on media coverage of military families in the book "A Battle Plan for Supporting Military Families." She previously worked for newspapers in Guam, Norfolk, Jacksonville, Fla., and Athens, Ga.



