U.S. military hospitals overprescribed opioids to patients with chronic pain from 2015 and 2017, a dangerous practice that put them at risk for addiction and overdose, according to the Department of Defense Inspector General’s Office.
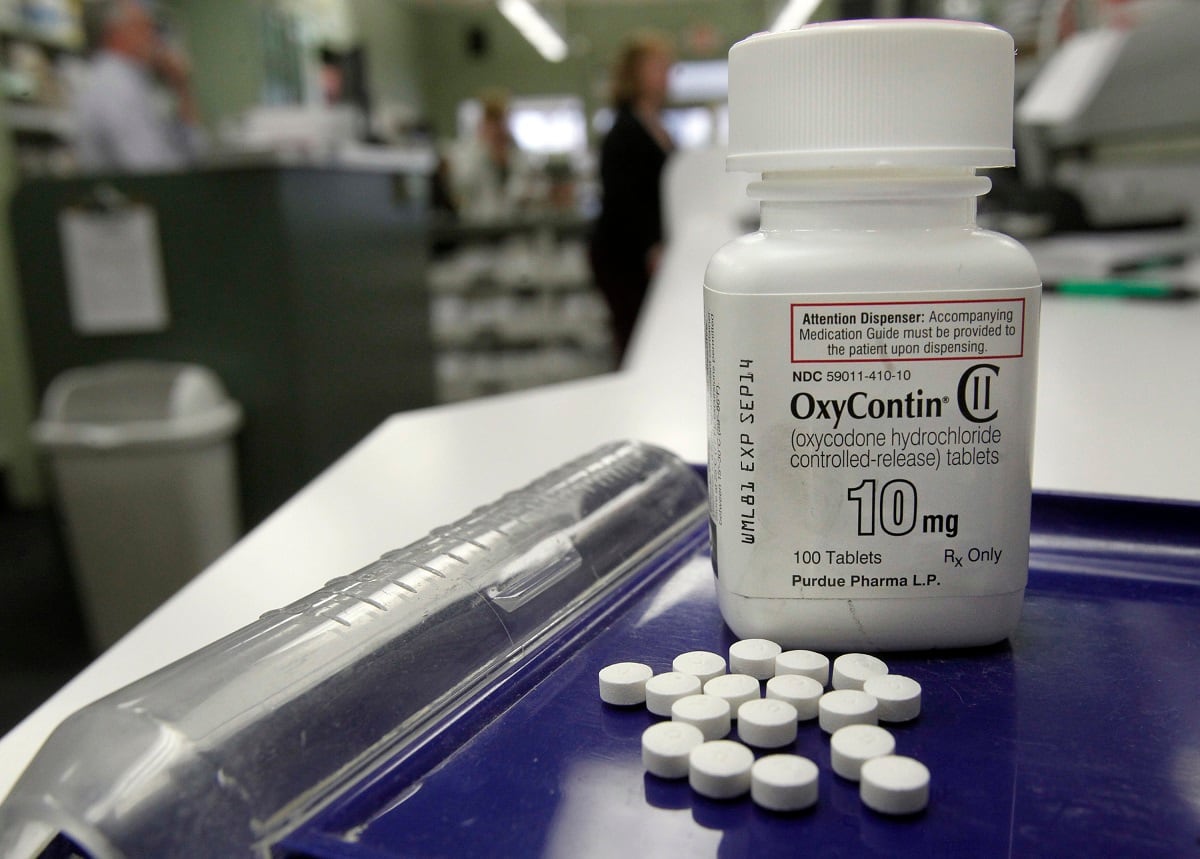
At three military medical facilities, some non-cancer patients were prescribed pills at more than five times the level recommended by the Centers for Disease Control and Prevention. In just one year, one patient in Alaska received 2,450 oxycodone tablets, while another was prescribed 4,700 over the course of two years.
Despite an opioid crisis that began more than a decade earlier, the Defense Department did not have policies or procedures in place to track patient prescriptions until 2017. That year, the Defense and Veterans Affairs departments issued joint clinical practice guidelines for physicians to consider when prescribing opioids and DoD implemented new systems for monitoring prescriptions.
RELATED
But the DoD OIG inspectors conducting the audit published Tuesday said that the staffs at the three military health facilities — Madigan Army Medical Center, Wash., Naval Medical Center Portsmouth, Va., and Joint Base Elmendorf-Richardson Hospital, Alaska — still “did not prevent providers from prescribing unusually high doses of opioids.”
At Madigan, they found one patient who was prescribed 12 pills per day of oxycodone, 12 pills per day of oxycodone-acetaminophen, 12 pills per day of hydromorphone, morphine sulfate, a fentanyl patch every three days and Ambien, a sleep aid that depresses the central nervous system and increases the risk for overdose.
“In 2015 to 2017, beneficiaries were allowed to receive unusually high amounts of opioids — for years in some cases — because the Defense Health Agency and the military departments did not identify and monitor beneficiaries who received over 90 [morphine milligram equivalents] per day,” the IG wrote.
The OIG conducted the audit to determine whether military hospitals overprescribed potentially addictive and deadly pain medications to patients with chronic pain not caused by cancer.
Inspectors sought to determine how well military physicians adhered to CDC recommendations that opioid prescriptions for chronic pain be limited to less than 90 “morphine milligram equivalents”, or MMEs, per day, roughly the equivalent of nine Vicodin or four tablets of sustained release oxycodone.
The IG found that providers weren’t restricted from prescribing high doses and weren’t questioned if they did. At one military hospital, inspectors spoke to a pharmacist who admitted that “many of the beneficiaries received unusual amounts of opioids” but would not go as far as saying that doctors had overprescribed the medications.
At another facility, a pharmacist said there wasn’t a “will to stop beneficiaries from getting their opioid medications.”
According to the Defense Department Psychological Health Center of Excellence, opioid prescription fulfillment has dropped across the military health system since 2007. But the study, released last October, also found that military retirees had a higher percentage of prescriptions over the CDC recommendations and were prescribed opioids more — 7 prescriptions per patient in 2017 — than active duty personnel, at 2 prescriptions per patient the same year.
At least four of the 15 patient records examined by the OIG were military retirees or dependents.
RELATED
The opioid crisis has largely been blamed for the increase in suicide and accidental deaths among veterans as well as civilians, and there is concern among veterans advocates that opioid prescriptions for injuries to active-duty service members may contribute to dependence on painkillers and potential addiction.
In 2011, veterans were twice as likely to die from an accidental overdose than non-veterans. But even though VA began cracking down on prescriptions from 2012 to 2015, overdose deaths have continued to rise with increased availability of illicit drugs such as heroin and fentanyl.
The Defense Department in 2017 identified 25,000 Tricare beneficiaries as having an opioid use disorder and 35 opioid-related deaths among active duty service members in 2015.
In the report, OIG recommended that the Defense Health Agency continue to monitor opioid prescriptions and hold physicians accountable for overprescribing them.
Also, because OIG was not able to obtain complete data on the number of beneficiaries in the system who have received prescriptions exceeding CDC recommendations, the staff recommended that the Pentagon improve its Military Health System Data Repository to ensure that all prescriptions are accurately recorded in the system.
DoD officials largely agreed with the recommendations but noted that it already implemented policies and procedures to identify, track and intervene if patients are prescribed inappropriate amounts of opioids.
They also noted that the new military electronic health records system, MHS Genesis, will improve prescriptions data.
Patricia Kime is a senior writer covering military and veterans health care, medicine and personnel issues.