Combat exposure puts U.S. troops and veterans at substantial risk for abusing prescription opioids and even heroin — more so than service members who deployed but never saw a firefight, according to a working paper published last month by the National Bureau of Economic Research.
In the study, entitled “Did the War on Terror Ignite an Opioid Epidemic?” economists with NBER, a non-profit that conducts economic research and disseminates it to policy makers, corporations and academia, determined that opioid abuse among combat-exposed veterans was 7 percentage points higher than among those who deployed but didn’t see combat.
Regarding heroin use, the authors noted that combat exposure also is associated with higher use rates, finding that combat-exposed personnel took heroin at more than 1 percentage point higher than fellow service members who never directly engaged with the enemy.
The results are the first to “estimate the causal impact of combat deployments in the Global War on Terrorism on opioid abuse,” the authors wrote.
Resul Cesur, associate professor of healthcare economics at the University of Connecticut, said he and his colleagues undertook the study to understand the impact of the United States’ post 9/11 war footing and its relationship to the veteran opioid epidemic.
They were motivated by a study they did in 2010 that examined the relationship between combat and the development of post-traumatic stress disorder and revealed that service members who had PTSD also reported taking opioids.
“We have an opioid epidemic in the military population. That is well known. And nearly three million deployed since 9/11, so what is the impact of this combat?” Cesur asked. “We wanted to know if it was driven by combat or by some other selection factor. For example, are people who are prone to opioid abuse drawn to enlist? ... Our evidence shows strong evidence that the reason why so many military people are using opiates is because they are exposed to combat.”
The authors said the differences appeared to be driven in part by the number of personnel wounded in combat and prescribed opioids.
About a third of opioid abuse among service members and veterans could be explained by a war injury, noted Cesur and his associates, Joseph Sabia, professor of economics at San Diego State University, and W. David Bradford, in the Department of Public Administration and Policy at the University of Georgia.
With heroin, nearly 58 percent of all abuse could be linked to a war injury, they found.
The heroin use research also found that while abuse of the illicit drug is rare in the U.S. military, Army and Marine Corps had the highest rates of use, the Navy came in third and Air Force had the lowest rate of heroin use.
Nearly 2.8 million U.S. service members deployed 5.4 million times to Iraq and Afghanistan.
While its unknown exactly how many U.S. troops and veterans misuse opioids or use heroin, in 2015, VA officials reported they had seen a 55 percent increase in opioid use disorders among veterans following combat operations in Iraq and Afghanistan, and in fiscal 2016, VA treated roughly 68,000 veterans for opioid addiction.
RELATED
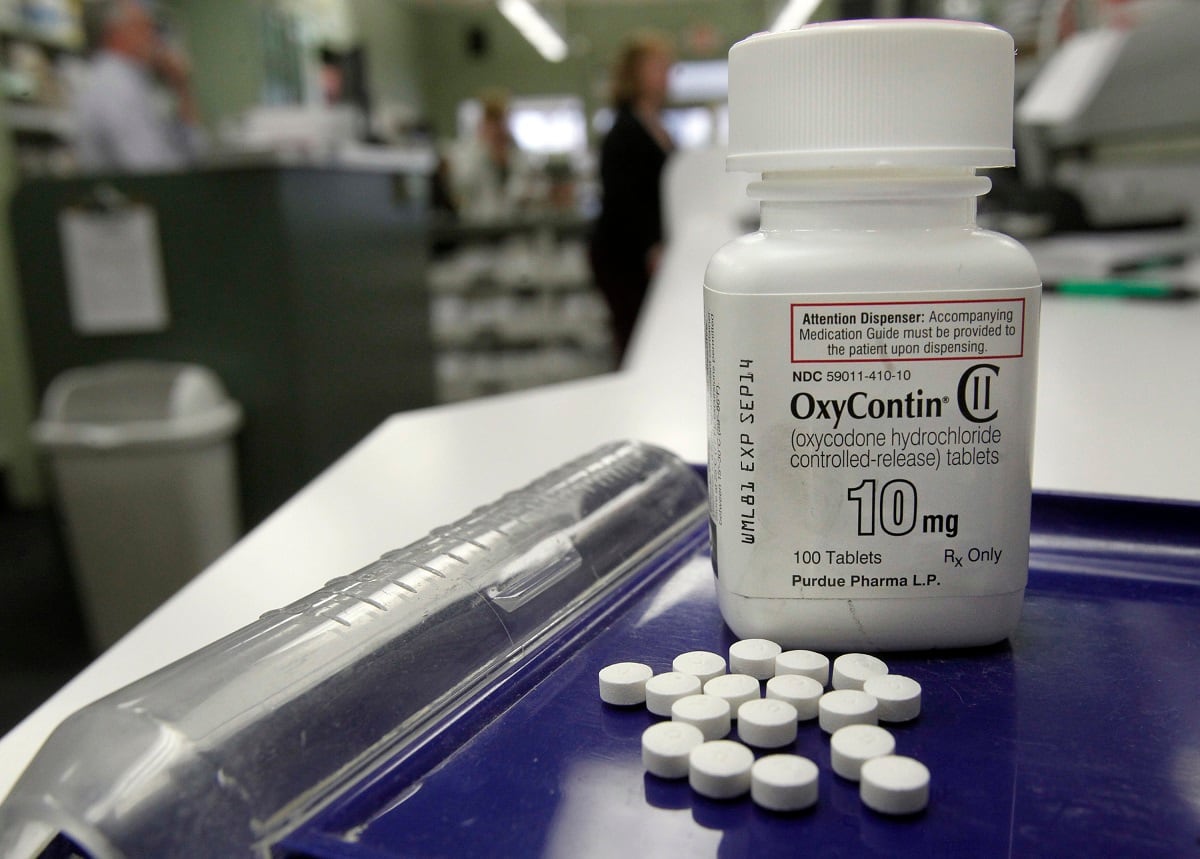
Between 2010 and 2016, 6,485 veterans in the VA health care system died of opioid-related causes.
Hardest hit has been the enlisted population, who tend to make up the bulk of those deploying, and who, according to previous research, tend to be more susceptible to combat related mental health conditions and substance use, the NBER study noted.
The study estimated that the economic impact of opioid addiction among service members is roughly $1 billion a year, and for heroin use, $470 million. The authors cautioned, however, that the cost likely is higher as U.S. troops and veterans tend to under-report problems with addiction or live in areas without access to therapy and medical treatment.
“These are likely to be the lower estimates of the economic impact of combat on treatment-related expenses,” Cesur said.
Both the Departments of Defense and Veterans Affairs have launched campaigns to curb opioid prescriptions and are conducting research to understand the scope of the problem within the military and veterans populations.
In 2010, DoD and VA issued new clinical practice guidelines aimed at reducing opioid prescriptions for pain other than end of live palliative care, and in 2013, VA launched an Opioid Safety Initiative aimed at encouraging pain management approaches that didn’t include opioids.
Opioid prescriptions have dropped by 40 percent at VA since 2012, the result of prescribing habits and greater reluctance of physicians to prescribe them.
This year, Air Force Capt. Carl Beyer discussed his work at the University of California Davis and David Grant U.S. Air Force Medical Center at Travis Air Force Base exploring the risk of opioid abuse among combat casualties at the Military Health System Research Symposium in Kissimmee, Florida.
According to Beyer, nearly 40 percent of all service members injured in combat were prescribed opioids at hospital discharge and a quarter continued to take them for a prolonged period of time following their discharges. Of those, nearly 7 percent developed opioid abuse.
The research may help develop strategies for prescribing pain medications to injured personnel and advance studies on alternatives or holistic therapies for managing pain, DoD officials said.
“The DoD and VA are really the only place in the United States where we have the long-term care of trauma patients under one health care system so we can do that long-term research. It’s really exciting,” Beyer told reporters at a press conference during the meeting.
RELATED

The NBER study concluded that combat exposure not only increases consumption of prescription narcotics and heroin, it also increases sedative and tranquilizer use for non-medical purposes and using opioids together with drugs like benzodiazepines, which also depress the central nervous system and increase the risk of overdose.
The authors added, however, that in states with medical marijuana is available, pain medication prescriptions, opioid-related hospitalization stays and age-adjusted opioid death rates have dropped.
“While marijuana legalization is certainly not a silver bullet, evidence that marijuana and opioids are substitutes suggests that access to medical marijuana may provide an alternative, less addictive, and less unhealthy means of treating pain,” they wrote.
“Opioids are deadly,” Cesur said. “There’s convincing evidence that use of medical marijuana may be an alternative.”
To draw their conclusions on the relationship between opioid use and combat exposure, the study authors used information from two major studies – the National Longitudinal Study of Adolescent and Adult Health and the 2008 Department of Defense Health and Related Behaviors Survey.
From the first study, they derived data from 482 male service members, nearly 13 percent of whom said they used prescription drugs for recreational or non-medicinal purposes. Using the second study, of 11,542 service men who reported being in combat, 9 percent said they used pain relievers for non-medical use and .6 percent reported using heroin.
Cesur said they used the data from the 2008 DoD study because its time frame correlated with results of the other survey and also, the DoD survey was conducted during a time frame when a large number of respondents had been deployed, either to combat or elsewhere.
Patricia Kime is a senior writer covering military and veterans health care, medicine and personnel issues.



