With Tricare open season approaching, it’s time to start thinking about whether you need to make changes.
Open season starts Nov. 14 and ends Dec. 13.
During that time, you can enroll in a health plan, change health plans or switch between individual and family enrollment. You can also remain in the plan you have, of course.
You aren’t required to make changes, but if you wish to, open season is the only time you can do it unless you have a qualifying life event such as moving, marriage, birth of a child or retirement from active duty. If you do have a qualifying life event, you have a 90-day period to make eligible enrollment changes.
If you’re not already in a plan and don’t enroll during open season, you’ll only be eligible for care at a military hospital or clinic — if space is available. Defense health officials advise that even if you don’t plan to make changes in your Tricare coverage for next year, you should check for any cost changes that could affect you.
Defense Health Agency officials released the 2023 Tricare Prime and Tricare Select fee schedule during the first week of November.
RELATED
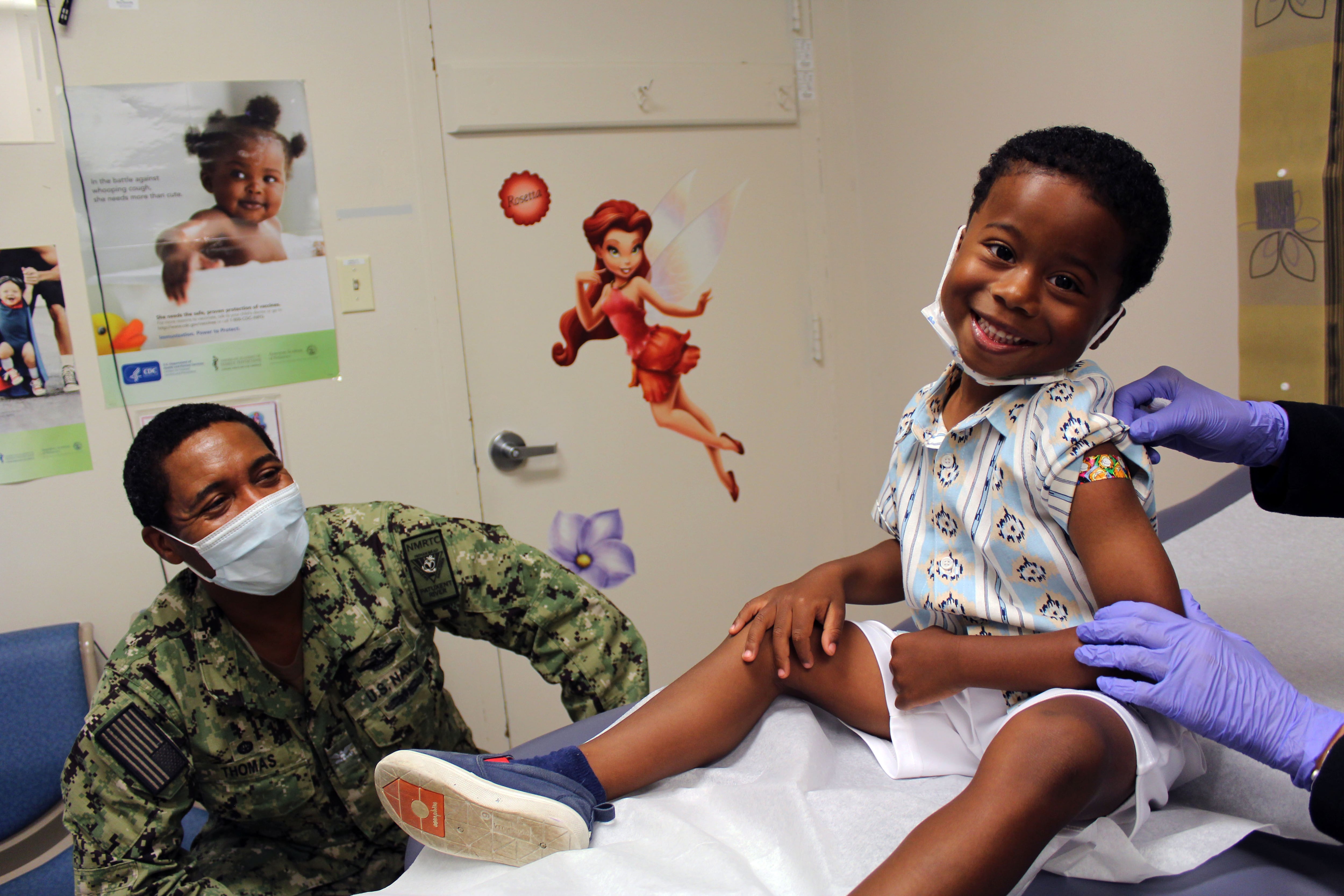
By law, DoD is required to raise certain beneficiary out-of-pocket cost shares by an amount based on the annual cost of living adjustment for retirees, which is 8.7% for 2023. Cost increases also reflect changes in the cost of health care services and drugs, and other factors, according to the Defense Health Agency.
There are also differences in some costs based on when the sponsor entered the military, which is required by law. Those who entered before Jan. 1, 2018, are part of Group A, while those who entered on or after Jan. 1, 2018, are part of Group B.

Who’s eligible to participate?
Anyone enrolled in or eligible for a Tricare Prime option (including the U.S. Family Health Plan) or Tricare Select, is eligible to participate in the open season.
Open season doesn’t apply to active duty members, who have full health coverage, and it doesn’t apply to retirees who are in Tricare for Life. Coverage is automatic if you have Medicare Part A and Part B.
Tricare Prime is a health maintenance organization-style plan in which you get most of your care from a primary care manager, with referrals required for specialty care. There is no deductible. Active duty service members, their family members and transitional survivors don’t pay enrollment fees or out-of-pocket costs for covered services. Retirees, their families and all others pay enrollment fees and out-of-pocket costs for covered services except for preventive care.
Tricare Select is a preferred provider organization-style plan in which you choose your Tricare-authorized provider and don’t have to get referrals for most services. There are deductibles, co-payments and cost-shares.
Those who have premium-based plans — Tricare Young Adult, Tricare Retired Reserve and Tricare Reserve Select — can buy these plans at any time. But those in Tricare Young Adult with the Prime and Select plan options can only change plans during an open enrollment season or qualifying life event.
For more information, visit the Tricare open season page.
Note: Make sure your information is current in the Defense Enrollment Eligibility Reporting System. If the information is wrong, you may not be able to use your Tricare benefit, and you could also miss enrollment deadlines.

New rates for Tricare premium-based programs
The rates have increased for the Tricare premium-based programs — Tricare Young Adult, Tricare Reserve Select and Tricare Retired Reserve — as determined earlier by the Defense Health Agency. Those increases take effect Jan. 1, 2023.
The new monthly premiums are:
♦ Tricare Young Adult: For TYA Prime, an increase of 11%, to $570 a month. For TYA Select, a 10% increase to $291 a month.
♦ Tricare Retired Reserve: An increase of 9%, to $549 a month, for the member only; and to $1,321 for the member and family.,
♦ Tricare Reserve Select: An increase of 4%, to $48 a month, for member only; and to $240 for member and family.
Pharmacy retail network changes
Tricare beneficiaries have the option of getting their medications through military pharmacies, retail network pharmacies and through the home delivery benefit. Active duty service members pay nothing for their prescription drugs when using these options. For others, the pharmacy costs for all these options will hold steady through Dec. 31, 2023.
The military pharmacy is still the lowest cost option for all military beneficiaries, because there’s no cost for covered generic and brand-name drugs at these pharmacies.
About 15,000 community and independent pharmacies left the Tricare retail pharmacy network on Oct. 24. Among the more than 40,000 pharmacies that remain in the network are CVS and Walgreens, as well as many grocery store pharmacies, wholesale warehouse stores and smaller chains, including some independent neighborhood pharmacies.
Defense Health Agency officials say that nearly 95% of beneficiaries will maintain access to at least two network pharmacies within 15 minutes from their home, and 99.8% will have access within 30 minutes.
You can find an in-network pharmacy using the Express Scripts Find a Pharmacy tool. If your pharmacy has left the network and you need to move your prescription, take your medicine bottles to another participating network pharmacy; that pharmacy will inform you of their process. You can also call your doctor’s office to ask for your prescription to be sent to the new in-network pharmacy, or call your new in-network pharmacy to ask them to transfer your prescription.
Other changes coming with the new year will affect those who rely on specialty medications for chronic, complex conditions such as cancer, rheumatoid arthritis, multiple sclerosis and other diseases. Beginning Jan. 1, Accredo will be the primary Tricare in-network specialty pharmacy, and beneficiaries must get their specialty medications from a pharmacy in the network.
Until this change, prescriptions for these specialty drugs were filled at a variety of locations, including a number of individual retail pharmacies, and through the Express Scripts mail-order pharmacy.
The Accredo service is already available for those who want to switch before Jan. 1.
Other benefits changes
There are a number of benefits changes in the Tricare program each year. Among those in 2022:
♦ Copayments or cost-shares are eliminated for long-acting, reversible contraceptive methods. Those include intrauterine devices, contraceptive shots and subdural contraceptive rods.
Anyone who was charged a copayment for any of these services after July 28 can submit a claim to their regional contractor for reimbursement after Nov. 1.
♦ Copayments and cost-shares are back for telehealth services. A temporary waiver of those costs that went into effect at the beginning of the COVID pandemic has expired, so patients now pay those costs, which are like in-person care costs and depend on the patient’s beneficiary category, health plan and appointment type.
Audio-only telehealth appointments became a permanent Tricare benefit in July 2022.
♦ Qualifying Tricare Prime or Tricare Select beneficiaries can enroll in the Tricare Childbirth and Breastfeeding Support Demonstration, which will run to Dec. 31, 2026. It will expand overseas in 2025. This demonstration project covers certified nonmedical labor doulas, lactation consultants and lactation counselors.
DENTAL
Families of active duty, National Guard and reserve service members— as well as guardsmen and reservists who aren’t on active duty — are eligible for the Tricare Dental Program, which requires separate enrollment.
Most retirees and their family members are eligible for dental and vision coverage under the Federal Employees Dental and Vision Insurance Program, or FEDVIP, which is administered by the Office of Personnel Management and also requires separate enrollment.
The rates will go up an average of 0.21% for dental in 2023.
The open season for FEDVIP this year is Nov. 14 through Dec. 12, which is one day shorter than the Tricare open season.
There are 23 dental plans offered by 12 carriers, seven of which provide nationwide coverage. The remaining five offer regional coverage.
If you’re already enrolled in a FEDVIP dental and/or vision plan and don’t want to make a change, your enrollment will automatically continue.
Vision
Those in the military community must be enrolled in a Tricare health plan to be eligible for FEDVIP vision coverage. Those eligible include active duty family members, retirees and their eligible family members, and Selected Reserve members and their families. There are 10 vision insurance plans available from five national providers.
There’s a bright spot in the vision coverage: Rates will decrease by an average of 0.41%.
Visit www.benefeds.com to enroll in FEDVIP and to get more information.
Federal Times staff reporter Molly Weisner contributed to this report.
Karen has covered military families, quality of life and consumer issues for Military Times for more than 30 years, and is co-author of a chapter on media coverage of military families in the book "A Battle Plan for Supporting Military Families." She previously worked for newspapers in Guam, Norfolk, Jacksonville, Fla., and Athens, Ga.





